Individual freedom and collective responsibility: yet another challenge for the health care system
The health and socio-economic situation of the last few years has brought each of us to question (again) the relationship between individual rights and freedoms and the social and collective responsibilities for our individual actions. Here we discover the views of Geert Demuijnck and Loick Menvielle, professors at the EDHEC Business School.
The relationship between individual and collective responsibilities has been discussed for centuries by thinkers in ethics, economics, and political science, and also in the health field. The unprecedented situation that all countries went through during the Covid-19 pandemic raised numerous questions about individual choices regarding vaccination and the contradictions that they generated.
The debate about the relationship between individual rights and collect responsibility is particularly complex. Rawls (1971) defined health as a “primary good” (1), that is, a good that everyone desires regardless of their ambitions and their personal plans. Contrary to other primary goods (such as certain material resources) health is a natural primary good, that is, it cannot be transferred from one person to another, unlike primary social goods. On the other hand, access to health care is obviously a social good: it is the social system that determines the access. The importance of health for everyone, and in turn, the importance of access to care, renders the reconciliation between individual liberty and collective responsibilities rather difficult.
What can we learn from international comparisons and how can we understand the tensions that occur daily inside the health sector? And what are their repercussions in the medium and long terms? Two EDHEC Business School researchers, Geert Demuijnck and Loick Menvielle, professors of Ethics and Marketing respectively, see their work as reflections that extend well beyond the crisis of the last three years. They shift questions about a health model within a distributive justice framework back to the centre of attention, concerning themselves with equity and equality of access to care.
Individual versus collective: international comparisons and a philosophical approach
Demuijnck describes the ethical debate about social justice and health as follows: “it’s a question of where to settle between libertarian approaches that advocate the maximum liberty for individuals and reject state paternalism, and those approaches that are more utilitarian or egalitarian, more concerned with public health and access to care for all, even if that implies a restriction of individual liberties”. He illustrates the point with an example: “We can have a libertarian system in which, as in some states of the US, bike helmets are not obligatory, but it will not be the community that pays for the health care in case of an accident. The doors to a hospital are not closed to bike accident victims, but it is their private insurance, or in the end, their own assets, that will pay the costs”.
The French system is at the other end of the spectrum, characterised by its refusal to discriminate in terms of access to health care on the basis of physical or social criteria, or individual behaviour. But even in a system such as this, for “this tension between the collective and the individual, usually latent, surges during an exceptional pandemic like the Covid-19 crisis, during which possibly risky behaviour can have multiplier effects”. Concretely, when this illness, which seriously affects older people, and the measures imposed on people (confinement, working from home, school attendance) affected those of all ages, the distribution of effort does not match the distribution of benefit: “the collective efforts and costs are akin, at such times, to the inter-generational solidarity actions and policies intended to benefit seniors – of which I am part – which older people do not always realise. We saw this, for example, in the cases of some older people refusing to be vaccinated” Demuijnck adds.
National and local approaches to “managing” this tension are varied. In Singapore, the non-vaccinated were obliged to pay their own health bills; in Austria, all residents over 18 (except pregnant women) were obliged to be vaccinated or pay a fine; in Germany, the chancellor tried, unsuccessfully, to make vaccination for the over-60s obligatory.
The vaccine raises the question of individual liberty versus collective responsibility in a particularly striking way. The usual criticism of “antivaxxers” was that they were engaging in risky behaviour while also expecting the collective to take care of them in case of a problem. But contrary to the example mentioned above, of the bike riders whose refusal to wear helmets poses a risk only to themselves, the non-vaccinated also affect – maybe above all - others, that is, the group of people who are at risk. Demuijnck says “what further complicates this is that the vaccine is not a 100% guarantee that someone will not either carry or spread the virus – it only reduces the probability – and we know that people are not always rational about probabilities”.
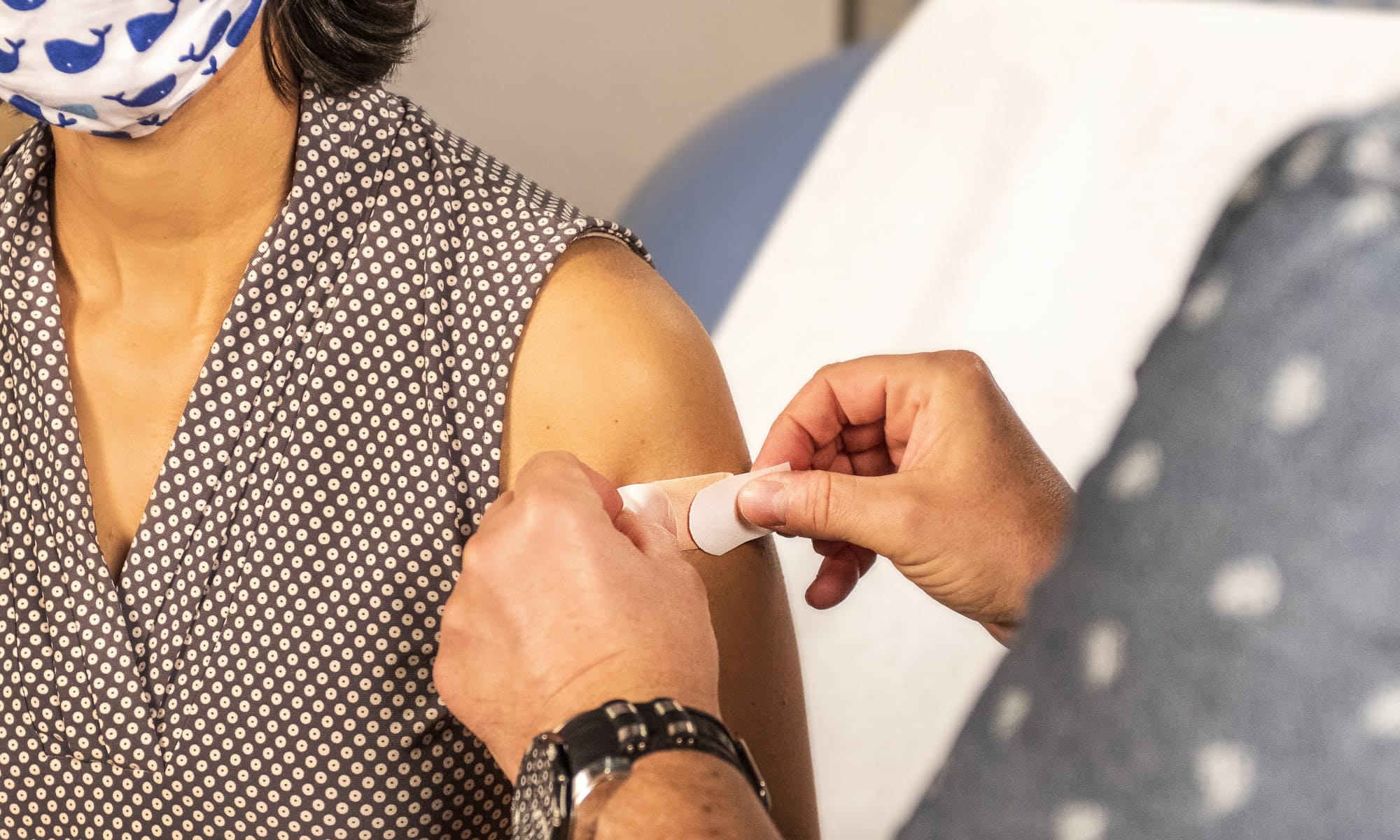
For Menvielle, it is essential to make a sideways step in order to understand the sources of these criticisms and their possible spread: “Intellectuals and politicians who defend individual liberties in the area of health, promote at the same time the idea that individuals are responsible for their own health, and that our health care system could treat people differently from each other - in terms of priorities, costs, level of care…” Demuijnck says: “Despite a health care system that is accessible to all, scientific studies are very clear about the link between socio-economic inequalities and health. Obesity, for example, is strongly correlated to the social situation of the individuals. To deny that, and to hold people “responsible” for their own health, by blaming them, can lead to the argument that some people deserve care (free and universal) and others do not.” (2)
How health professionals experience living with the contradictions
While people are not responsible for all the factors (genetic, social, demographic…) that determine their health, they can be held responsible for their choice not to be vaccinated. The sum of individual choices also has consequences for the structures, especially hospitals, particularly in recent years. Menvielle reminds us that “at the beginning of the epidemic in mid-January 2022, the proportion of patients in intensive care after they had caught Covid-19 was one in two, oscillating between 75% and 125% of intensive-care bed capacity”. (3) This affected the management of patients suffering from chronic illnesses and other problems, such as stroke. As if France had become a sort of “giant hospital”, we absorbed statistics, terms, and images about vaccinations and contaminations. But the accumulation of macroeconomic data seemed at times to have displaced the key issue of the concrete consequences of the refusal, by hundreds of thousands of people, to be vaccinated.
Menvielle explains: “The health professionals were brutally confronted by this question, because every day, for months, they had to struggle with a real paradox: caring for those who had been vaccinated, but with a team that either remained the same size or was reduced and being obliged to reprogramme dozens of other procedures.”
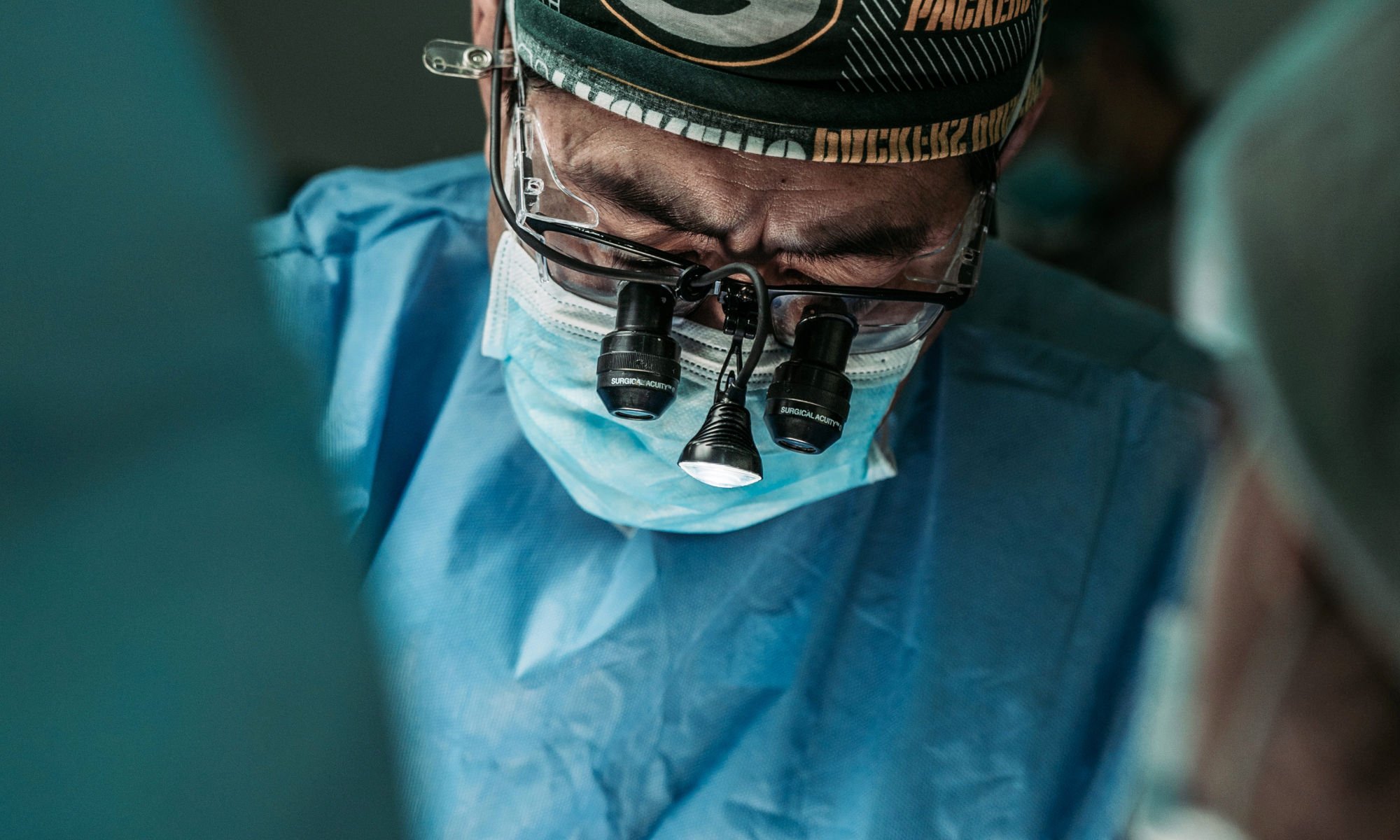
What does this situation tell us? Accommodating individuals’ choices not to be vaccinated and at the same time care for everybody comes at a cost. Demuijnck notes that “in France, the debate never really took place. Everyone was provided for and the non-vaccinated were free to make their choice without being too stigmatised for the irresponsibility of that choice – apart from Emmanuel Macron’s infamous stated desire to “piss off the non-vaccinated”, which was undoubtedly counter-productive. While the health system weathered the storm, the profound effects of the crisis are not yet over.
2020-2023: repercussions for society, today and tomorrow
Everyone is conscious of the fact that the effects of certain social divisions that deepened during the pandemic will be felt for several years to come. “Doubts about the political authorities, which are confused with the health system in many citizens’ minds, will certainly affect health care in the future” Menvielle says.
Consequently, thousands of people, especially those who were already insufficiently monitored and treated, risk further delaying, even abandoning, their medical care. Demuijnck asks: “rather than compelling, or charging, or using other ‘sticks’, how can we work collectively to reaffirm the power and the legitimacy of what scientists have to say? When we read the extraordinary, even conspiratorial, arguments of the antivaxxers, we cannot help but question the role and the impact of social media networks compared with more traditional channels”.
There is no shortage of ways to bring new perspectives to bear on these subjects: making a critical review of the choices made during the period in relation to the invisible mechanisms of our system, by hypothesising, for example, that the positions of the non-vaccinated were as often a consequence as a cause; moving away from the stigmatisation in order to reconstruct confidence and to recognise our capacity to take into account individual paths and situations within the collective; affirming that individual liberty and personal responsibility can be complementary; and insisting that holding individuals entirely responsible for their situation and their choices is an argument built on potentially deleterious shifting sands.
Références
(1) Rawls J. (1971). A theory of justice. Cambridge, Massachusetts : The Belknap Press of Harvard University Press.
(2) See e.g. the work of Michael Marmot in the UK, or Thierry Lang in France, and, in a broader perspective, Michael Sandel’s must-read The Tyranny of Merit.
(3) Office des publications de l'Union européenne (Janvier 20, 2022). Part des patients actuellement en réanimation ou soins intensifs des suites du COVID-19 sur la capacité totale de lits disponibles en France du 19 mars 2020 au 19 janvier 2022.
Crédits
A. Photo de mauro mora sur Unsplash
C. Photo de JC Gellidon sur Unsplash


![[#dataviz] Santé connectée et IA : quelles tendances pour 2026 ?](/sites/default/files/styles/actu_850_480/public/2026-03/2026-03-header-dataviz-vox-sante-connectee.jpg?itok=FN6aCgt6)

